Type 2 Diabetes
Type 2 diabetes (T2D) is a chronic condition that affects how your body manages glucose.
Glucose is the scientific name for sugar, an important source of energy for your body. Your system relies on a hormone called insulin to move glucose from the bloodstream into your cells.
In type 2 diabetes, the body makes insulin. But it doesn’t respond to it as effectively as it should. Over time, insulin production may also decline.
Get expert type 2 diabetes treatment in San Antonio.
What Causes Type 2 Diabetes?
The hallmark of T2D is insulin resistance. This means that your cells don’t respond to insulin the way they should.
Early on, your pancreas compensates by making more insulin. Eventually, that compensation becomes harder to sustain. Blood sugar levels begin to rise. When insulin resistance develops:
- Glucose stays in the bloodstream longer
- Cells don’t get the energy they need
- The pancreas works harder to keep up
Over time, this imbalance can quietly affect the health and function of your:
- Blood vessels
- Nerves
- Organs
Who Develops Type 2 Diabetes?
Type 2 diabetes is more common in adults. But it can occur at any age. Risk factors include:
- Family history of diabetes
- Weight gain, particularly around the abdomen
- Limited physical activity
- History of gestational diabetes
What Are the Symptoms of Type 2 Diabetes?
T2D often goes unnoticed at first, with symptoms developing later, such as:
- Fatigue
- Increased thirst or urination
- Blurred vision
- Slow-healing wounds
- Tingling or numbness in the feet
How Is Type 2 Diabetes Diagnosed?
T2D is often found through routine blood work, not because someone feels unwell. Tests that are used include:
- Hemoglobin A1C: A blood test that shows your average blood sugar over the past few months
- Fasting blood glucose: A blood sugar test done after you haven’t eaten for several hours
- Oral glucose tolerance test: A test that checks how your body handles sugar after you drink a sweet liquid
- A random blood glucose test: Done at any time of day to show your blood sugar level at that moment
How Is Type 2 Diabetes Treated?
Care for T2D often starts with simple, everyday changes. For most people, lifestyle changes are a starting point, beginning with:
- Nutrition adjustments
- Increased physical activity
- Weight management strategies
These changes can improve insulin sensitivity. In some cases, they can significantly slow disease progression.
If lifestyle changes aren’t enough, medications may be added to:
- Improve how the body responds to insulin
- Reduce glucose release from the liver
- Help regulate blood sugar after meals
Some people eventually require insulin, but this often happens later on, not at diagnosis.
Advanced Glucose Monitoring
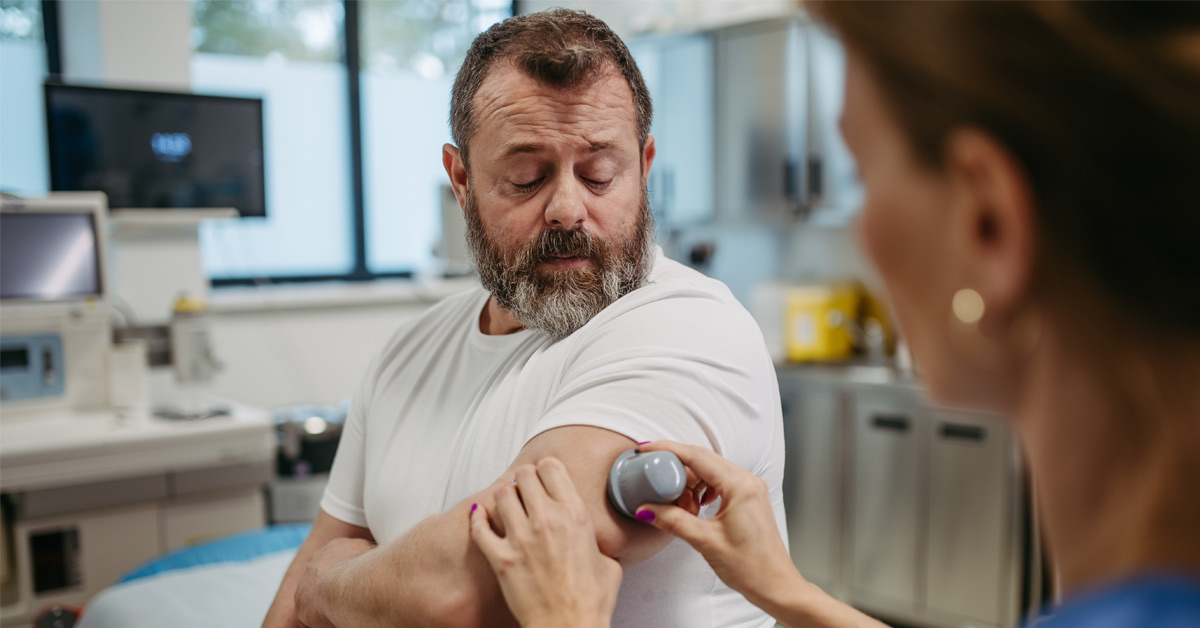
Some people with type 2 diabetes benefit from added testing and technology to better understand their blood sugar. Continuous glucose monitors (CGMs) track blood sugar day and night. They show how food, activity, stress, sleep, and medicine affect glucose levels. This information helps people spot patterns and make better daily choices. Some CGMs are worn on the skin, while others, like the Eversense CGM, are implantable and provide long-term glucose tracking.
Are There Ways to Diagnose and Prevent Complications?
Yes. Finding problems early is an important part of type 2 diabetes care.
Nerve health
Type 2 diabetes can damage nerves over time. SudoScan is a quick, noninvasive test that checks early nerve changes, often before pain or numbness begins.
Circulation
Type 2 diabetes can reduce blood flow to the legs and feet. The ankle-brachial index (ABI) compares blood pressure in the arm and ankle to help detect circulation problems early.
How Is Nerve Pain Managed?
In some people, long-standing type 2 diabetes leads to painful diabetic neuropathy. Symptoms may include:
- Burning
- Tingling
- Numbness
- Shooting foot or leg pain
Treatment focuses on symptom management. This may include medications.
Type 2 Diabetes FAQs
1. What does it mean to live well with type 2 diabetes?
Successfully living with T2D is all about managing it over time. Small, steady steps can make a big difference. Watching for early warning signs and making simple lifestyle changes can help slow the condition and lower the risk of complications.
2. When should I contact my doctor or seek medical care?
You should reach out for medical help if you notice:
- Blood sugar levels that stay high despite treatment
- Signs of dehydration, such as extreme thirst or very little urination
- Worsening numbness, pain, or wounds on the feet that aren’t healing
- Confusion or changes in alertness
3. Can type 2 diabetes be reversed?
Type 2 diabetes can sometimes improve. In some people, blood sugar returns to a healthy range. This is called remission, not a cure.
Healthy eating, weight loss, exercise, and medicine can help. Some people may not need medicine for a while. A doctor can help you make the best plan.










